As our ability to treat and manage chronic medical conditions improves, we will see a greater number of our patients manifesting physiologic as well as pathologic changes associated with aging. The objective of this article is to provide a brief overview of physiologic changes seen in the respiratory system with aging, and to discuss commonly encountered challenges associated with the management of pulmonary disorders in the elderly patient population. PubMed was searched, using the keywords “aging” and “elderly”, combined with “asthma”, “COPD”, and “lung cancer”. The references of appropriate papers were then reviewed to obtain further relevant information.
Aging is a complex biologic process that is characterized by irreversible functional and anatomic changes in the body, resulting in increased susceptibility to disease processes. The respiratory system undergoes multiple changes with aging, which increases the frequency of commonly seen symptoms, such as cough, rhinitis, and dyspnea. As people age, nasal passages become less cartilaginous resulting in overall decreased patency. Similar changes in the collagen support network occur at the level of proximal and distal airways, which causes enlargement of alveolar ducts leading to air trapping and loss of surface area for gas exchange.1 The efficiency of gas exchange is further affected by a decrease in the diffusing capacity of carbon monoxide at an approximate rate of 5% per decade.2 There is a loss in contractility of intercoastal and diaphragmatic muscles, resulting in overall decreased expansion of airways and increased atelectasis.3 Due to decreased chest wall muscle strength, the cough becomes less effective. There is also a decrease in the effectiveness of mucociliary clearance with age.4 The rate at which these changes occur is influenced by genetic predisposition as well as environmental factors, like cigarette smoking. The decrease in the elastic recoil and compliance seen in older patients contributes to a diminished respiratory reserve, which then contributes to acute conditions, such as pulmonary edema, pneumonia, and bronchospasm.5 Clinicians should keep these physiologic changes in mind while evaluating older adults presenting with pulmonary-related symptoms and consider them in diagnosis and management.
Evaluation of commonly reported respiratory symptoms in the elderly
The most commonly reported pulmonary symptoms in the elderly include dyspnea, cough, and decreased exercise tolerance. These symptoms can be caused by a variety of pulmonary, as well as non-pulmonary, conditions. Cough with sputum is reported by up to 27% of elderly patients and is associated with increased mortality.6 Similarly, dyspnea is highly prevalent in the elderly, and is reported by approximately 30% of individuals >65 years of age.7 Due to the high likelihood of multiple comorbid conditions, all elderly patients presenting with symptoms of dyspnea and cough should be approached with a broad differential in mind.
Acute onset of dyspnea in the elderly, especially when associated with changes in vital signs (tachycardia, tachypnea, or fever), is best evaluated in the emergency room. Chronic dyspnea requires a stepwise approach to diagnose the underlying condition. After obtaining a thorough history and physical examination, a chest x-ray should always be considered as the first diagnostic tool. Chest x-rays are readily available, cost effective, and can provide valuable information in a variety of pulmonary conditions. Infiltrates may point towards pneumonia; findings of edema are suggestive of heart failure; prominent interstitial markings can be seen in interstitial lung disease; and hyperinflation suggests chronic obstructive pulmonary disease (COPD). However, further evaluation with pulmonary function testing, echocardiogram, and chest computed tomography (CT) scan is often needed for a complete evaluation of chronic dyspnea.
Asthma
Asthma is a chronic inflammatory condition characterized by reversible airway obstruction resulting in recurring and variable symptoms of cough, wheeze, shortness of breath, and chest tightness. Asthma remains a highly prevalent and deadly disease in patients >65 years old. The prevalence of self-reported asthma in this age group is 6.8% and the lifetime prevalence is estimated to be 13%.8,9 Compared with younger patients, asthma in older patients is associated with higher mortality, more severe exacerbations, and longer hospital stays.10 These trends can be explained by increased burden of comorbid conditions, higher rates of misdiagnosis and underdiagnosis,11 decreased perception of asthma-related symptoms,12,13 and underutilization of guideline-directed management.14 The two distinct types of asthma phenotypes described in older patients include late-onset and longstanding (Table 1). Late-onset asthma usually presents in middle age, is less commonly associated with atopy and positive family history, and is more frequently associated with tobacco use and obesity.15
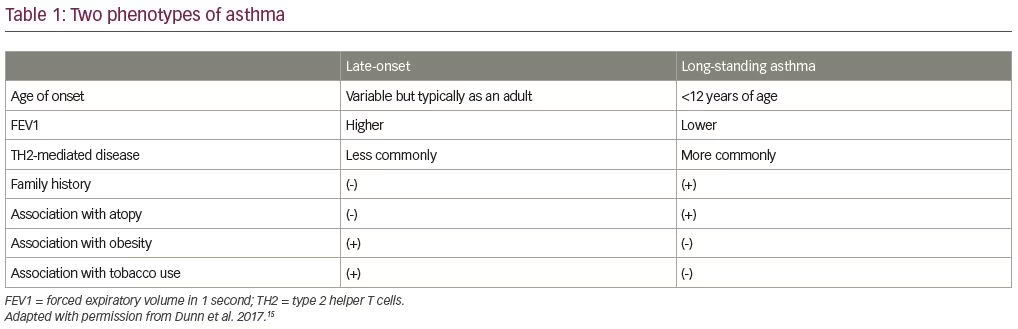
Asthma should be suspected in patients presenting with symptoms of bronchoconstriction, including cough, shortness of breath, wheeze, and chest tightness. Frequently, symptoms are subtle and easily misdiagnosed or overlooked. Diagnosis of asthma in older patients requires a careful approach that is centered around ruling out other causes of dyspnea and wheezing, including COPD, bronchiectasis, constrictive bronchiolitis, and congestive heart failure. In one study, it was reported that asthma in older patients can be misdiagnosed as COPD in up to 20% cases.11 Compared with COPD, asthma in older patients is more likely to have increased serum and sputum eosinophils, greater bronchodilator response, and association with atopic conditions, while the presence of hypoxemia, heavy smoking history, and hyperinflation of lungs points towards COPD.16,17
Despite these well-defined differences, the diagnosis of asthma remains a challenging issue. An improvement in forced expiratory volume in 1 second (FEV1) of at least 12% after receiving short-acting bronchodilator is helpful in establishing a diagnosis, but this can also be present in COPD. While interpreting the results of spirometry in the elderly, it is essential to use age-adjusted values due to an accelerated decline in FEV1 as a result of aging.18,19 Frailty and cognitive impairment in the elderly can increase the challenges of obtaining accurate results using spirometry.20–22 Provocation testing using methacholine can be used in older patients with normal baseline spirometry; however, it should be noted that there is conflicting evidence regarding increased airway hyperresponsiveness due to aging itself, which may lead to false-positive results.23–25 Based on a study by Columbo and colleagues, there was no correlation between exhaled nitrous oxide and spirometric values.26 However, more recent literature showed a correlation of fraction of exhaled nitrous oxide with asthma symptoms and a previous diagnosis of asthma.27 The utility of measuring the fraction of exhaled nitrous oxide in older patients with asthma remains unclear and requires further research.
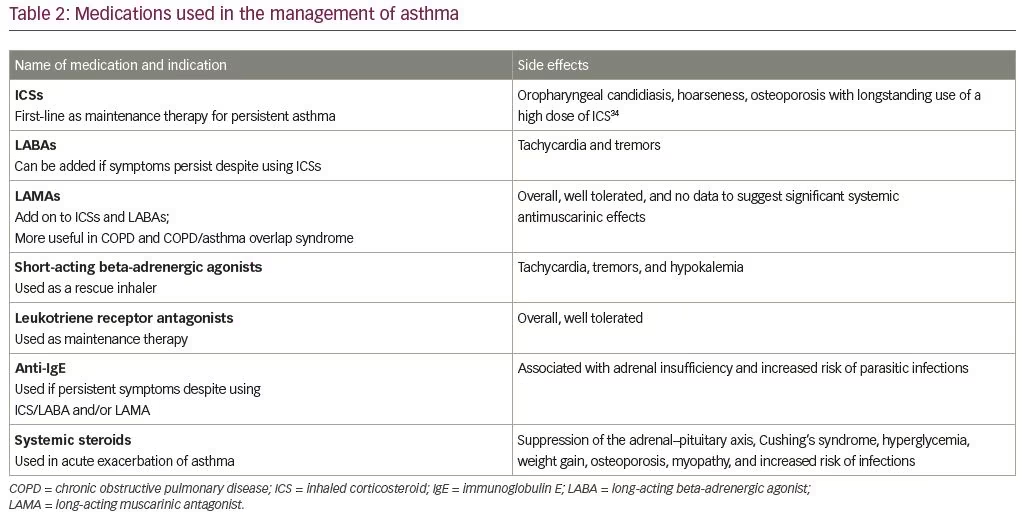
There are no age-specific guidelines for the treatment of asthma. The goal of asthma management is to control symptoms, prevent acute exacerbation, and reduce the need for hospitalization. Treatment of asthma in older individuals should be tailored using established guidelines.28 Common classes of medications and their side-effect profiles are listed in Table 2. Inhaled corticosteroids are an important component of asthma management, but they are significantly underutilized in older adults.14 Older patients with asthma are at higher risk of treatment failure compared with young patients.29 There are multiple challenges associated with the treatment of asthma in older patients including the decreased perception of asthma symptoms,12,13 lower adherence to medications due to cognitive impairment,30 poor inhaler techniques,31 and higher risks of side effects.32,33
Chronic obstructive pulmonary disease
COPD is defined by the Global Initiative for Chronic Obstructive Lung Disease (GOLD) as “A common, preventable, and treatable disease that is characterized by persistent respiratory symptoms and airflow limitation that is due to airway and/or alveolar abnormalities usually caused by significant exposure to noxious particles or gases.”34 It is reported to be the fourth leading cause of mortality in the USA,35 and is associated with aging,36 inhalational exposure to tobacco smoke, occupational dust and chemicals, and air pollution.37 There is a high burden of comorbid conditions in older patients with COPD, which creates multiple diagnostic and management challenges.38–40 Older patients with COPD may attribute their symptoms of COPD to comorbid conditions like congestive heart failure, muscle weakness, physical deconditioning, or age-related changes.35 When evaluating older patients with COPD, it is important to know that these patients may use different wording to describe dyspnea like “awful,” “terrifying,” or “frightening” as opposed to patients without COPD.41
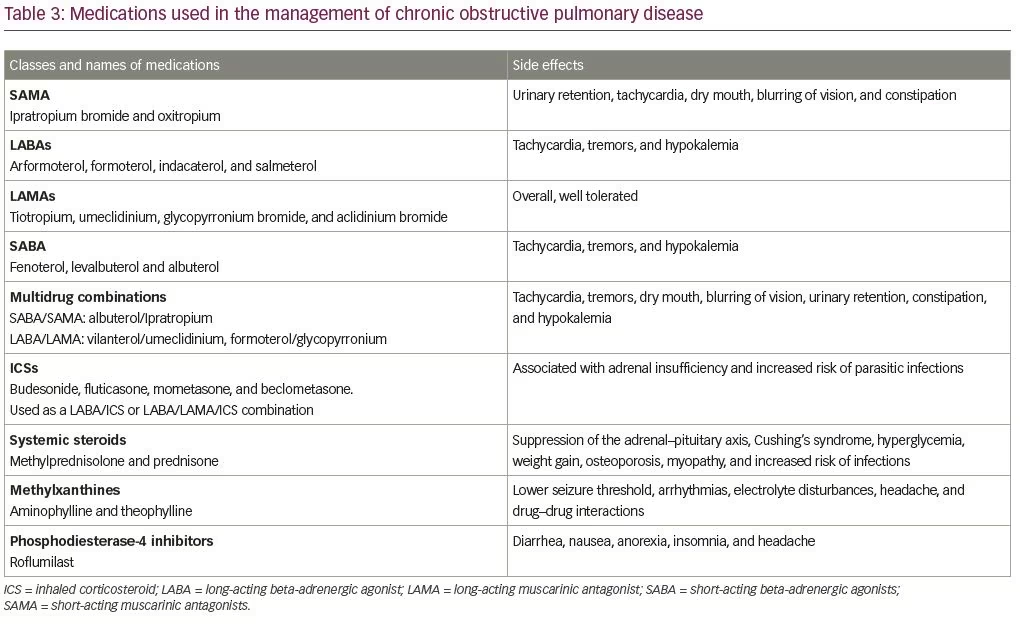
As discussed above, there are several age-related, unavoidable structural changes in the lung that lead to a decrease in lung functions. This creates an issue of overdiagnosis of COPD in older patients.42,43 It was found that up to 35% of healthy and asymptomatic patients aged ≥70 can be diagnosed as COPD stage I based on GOLD definitions.42 In order to reduce the risk of overdiagnosis of COPD in older patients, the American Thoracic Society and European Respiratory Society recommend using less than the fifth percentile of the normal distribution of FEV1 and vital capacity ratio as the cutoff for diagnosing of COPD.44 There are no age-specific guidelines for COPD in older patients, and management should be guided using the most recently published GOLD guidelines.34 In addition to inhaler therapies, long-term oxygen use, smoking cessation, and pulmonary rehabilitation are integral components of management. Common medications used to treat COPD are listed in Table 3. Inappropriate inhaler techniques, non-adherence to medications, and increased risk of medication-related side effects are common challenges with the treatment of COPD in older patients.45
There are positive outcomes associated with the use of long-acting inhaled bronchodilators in COPD including reduced symptoms,46 fewer acute exacerbations, and improvement in spirometric values.47 Inhaled corticosteroids, when used in combination with inhaled bronchodilator therapy, are associated with a decrease in emergency visits, need for hospitalization, and intubation.48–51 Non-pharmacologic interventions, such as smoking cessation, oxygen therapy in patients with resting hypoxia, and pulmonary rehabilitation are associated with improved survival and quality of life in patients with COPD.52,53
Lung cancer
Lung cancer is a common malignancy and one of the leading causes of cancer-related deaths in the USA. It is diagnosed in approximately 230,000 patients and results in 135,000 deaths annually. Despite the improvement in mortality in recent years, lung cancer has caused more deaths than colorectal, prostate, breast, and brain cancer combined.54 Its incidence increases with age and peaks between the ages of 59 and 75 years.55,56 Cigarette smoking is the number one risk factor for lung cancer and is associated with up to 90% of lung cancer cases.57 This risk is significantly reduced with the cessation of cigarette smoking with the greatest reduction in risk when cigarette smoking is stopped prior to age 30 years.58 Cigar and pipe smoking are also associated with an increased incidence of lung cancer, but the risk is substantially less than cigarette smoking.57 Other risk factors for the development of lung cancer include radiation therapy;59 history of pulmonary fibrosis;60 human immunodeficiency virus (HIV) infection;61 and exposure to secondhand smoke, radon, asbestos, arsenic, nickel, chromium, and polycyclic aromatic hydrocarbons.57
The majority of lung cancers are advanced at the time of diagnosis and it is common for patients to have metastatic disease at the time of presentation.62 The most common symptoms of lung cancer are cough, weight loss, and dyspnea. Other less common symptoms include chest pain, hemoptysis, bone pain, and hoarseness.63 Most cases of lung cancer can be broadly categorized into non-small cell lung cancer (NSCLC) and small cell lung cancer (SCLC), based on histologic subtype. These drive the decisions regarding management and prognosis. The treatment of lung cancer should not be solely based on the patient’s age, but it is important to take age-related changes in functional status and cognition into account when formulating a management plan. There are data that demonstrate that older patients treated with surgical resection for lung cancer had comparable outcomes to younger patients.64,65 Despite this, older patients are less likely to receive appropriate therapy compared with young patients.66
The treatment of lung cancer in older patients should be done in line with published guidelines of the American College of Chest Physicians. Surgical resection is usually the most suitable treatment option for patients with early NSCLC. Patients who are deemed nonsurgical candidates, or those with advanced disease, may be treated with radiation therapy, chemotherapy, and/or immunotherapy. Chemotherapeutic options are associated with a wide variety of short- and long-term toxicities in older patients;67 however, there are data suggesting that chemotherapy for NSCLC and SCLC have acceptable safety and outcome profiles in older patients.68,69
It is common for lung cancer patients to have advanced disease at the time of initial presentation,62 which leads to overall poor outcomes. Thus, in recent years, there has been intense research on the development of screening models for lung cancer. Several modalities for lung cancer screening have been investigated, including sputum cytology, chest radiograph, and low-dose CT scan. The National Lung Cancer Screening Trial (NLST) was a multicenter, randomized control trial that compared low-dose CT scan with chest radiograph in asymptomatic adults aged 55–74 with >30 pack-year smoking history. It included current as well as former smokers who quit within the past 15 years. NLST showed a significant reduction in mortality in patients who underwent low-dose chest CT for the detection of lung cancer.70 Sputum cytology and chest radiographs are not recommended for lung cancer screening.70–72 Based on the published data supporting the use of low-dose chest CT for lung cancer in the high-risk patient population, the United States Preventative Task Force implemented guidelines recommending annual screening for lung cancer with a low-dose CT scan for adults aged 55–80 who have a 30 pack-year smoking history and currently smoke or have quit within the past 15 years. Screening is not recommended for patients with substantially limited life expectancy, contraindication, or unwillingness to undergo curative lung surgery.
Conclusion
Despite recent advances in the field of pulmonary medicine, there is still room for improvement in the diagnosis and management of common pulmonary diseases in the older patient population. When evaluating older patients, clinicians should be mindful of physiologic and anatomic changes associated with aging. The burden of coexisting medical conditions is frequently much higher in older patients and many of these comorbidities can mimic pulmonary disorders. The evidence suggests that pulmonary diseases are often misdiagnosed as well as inappropriately treated in elderly patients. Both asthma and COPD are common in the elderly and are associated with increased mortality. Diagnosis is often challenging due to coexisting medical conditions that may present with similar symptoms. In addition, changes in cognition and pulmonary physiology may limit the utility of commonly used testing tools, like pulmonary function testing. Similar to COPD, the incidence of lung cancer increases with age. It is often diagnosed late, and older patients are less likely to receive appropriate and timely management compared with younger patients. More research is needed to better identify these challenges and issues in the management of pulmonary disorders in elderly patients. It is also important to educate medical practitioners on this topic so that appropriate and evidenced-based patient care is provided to older patients.






