Epidemiology
Strains of Mycobacterium tuberculosis (M. tbc) are able, like other bacteria, to develop resistance against antibiotics. The first observations were published shortly after the introduction of streptomycin and were the basis of the current recommendation of combining several antibiotics for the treatment of tuberculosis (TB).1 Rigorous application of this principle could have possibly prevented the development of drug resistance. In spite of this, drug resistance against the most active antibiotics increased progressively and is currently a widespread phenomenon. Apart from resistance against single drugs, resistance against the two most active anti-TB drugs, isoniazid and rifampicin, known as multidrug resistance (MDR-TB), has increased and new forms of resistance have emerged, like the resistance against isoniazid, rifampicin, injectable drugs and quinolones, known as extensively drug-resistant strains (XDR-TB).
The latest reports from the World Health Organization (WHO) estimate the number of MDR-TB to half a million cases, of which 10 % are XDRTB, a large part being left untreated, with a high death burden.2 In some regions of the world or in some at-risk populations, like gold miners in South Africa, the rate of MDR-TB is increasing rapidly, particularly in previously treated cases, in spite of the fact that the global incidence rate in the same population had decreased during the same time period.3 Recent reports reveal alarming levels of drug-resistant TB in many Eastern European regions,4 such as Belarus, where the rates reach 35.3 % in new patients and 76.5 % among previously treated cases5 or in Ukraine, where the association with HIV seems to increase the problem.6 In Russia, if the current trends continue, the incidence of drug-resistant TB could be higher than the incidence of drug-sensitive TB within the next few years.7 Prisons seem to be places where the incidence of TB (including drug-resistant forms) is particularly high.7,8 In China, a recent survey concluded that the proportion of MDR-TB cases among new and previously treated patients is 5.7 % and 25.6 %, respectively, and the total number of MDR-TB cases is about 110,000.9 The increase in drugresistant TB is also observed in children in some regions of the world.10
Risk Factors for MDR-TB
Most surveys report an association between previous treatment for TB and high rates of drug resistance.11,12 The prevalence of MDR-TB is higher among patients who were already treated for TB and failed or recurred, but this group represents only a minority among all cases of TB. In absolute numbers, the majority of cases is observed in new patients, who never received a treatment before and who were contaminated by a patients harbouring a resistant strain.13 As a consequence, in some regions of the world, new patients are at high risk of having MDR-TB even in the absence of previous treatment.
Apart from close contact with a patient with drug-resistant TB, other factors associated with the presence of MDR-TB are migration, young age and HIV.14
One particular cause seems to be the induction of resistance by insufficient bioavailability of some anti-TB drugs such as rifampicin.15 Low serum levels of anti-TB drugs, which are observed in some patients,16 may induce the development of resistance against one or several drugs. Some studies have confirmed that patients with a low serum level of the first-line anti-TB drugs have a worse outcome than patients with a level within the expected range.17 This may also explain why some patients develop a drug-resistant form of TB in spite of full adherence to a correct treatment.18,19 One may suspect that drugs of low quality or insufficient bioavailability may contribute to the creation of drug resistance. How important this phenomenon may be in the progressive extension of MDR-TB in some regions is unclear. Studies are ongoing to decide if the recommended dose of rifampicin will have to be changed in the future.20
Why is MDR-TB Increasing in Some Regions of the World?
There are many reasons for the increase of MDR-TB and XDR-TB worldwide, but they all have one point in common: there was some error along the chain of management, inducing a mutation in a strain of sensitive mycobacteria and the selection of mycobacteria that have become resistant to one or several antituberculous drugs, which will progressively replace the sensitive bacteria.21 Among the usual causes are inappropriate treatment of mycobacteria with an undetected resistance against a single drug, use of drugs of bad quality, insufficient drug dosage, changes in drug schedule or dosage and addition of a single drug to a failing regimen. Retreatment of patients with a recurrent episode of tuberculosis with the same drugs as for the first episode, without appropriate drug susceptibility testing (DST), is a possible cause of amplification of the drug-resistance pattern and transformation of a strain with single drug resistance to MDR-TB. This can happen even under normal programmatic conditions, if the drug sensitivity testing is not performed in suspect cases.22,23 Patients with an unsuspected drug resistance who are not cured at the first treatment attempt have a high risk of developing further resistance and harbour an MDR-TB strain.24–26 This is the reason why the ancient recommendation of WHO to use a retreatment regimen containing the same first-line drugs in addition to streptomycine, which has proven successful in settings with a low frequency of drug resistance,27 has been put into question28 and is now no more valid.29 Furthermore, some strains, like the Beijing genotype, seem to mutate more rapidly and be more virulent so that in some regions they progressively replace the other strains.30
The practical issue is that in many settings, if the DST of the strain are not performed rapidly (which is the norm in many regions lacking proper laboratory equipment), patients with MDR-TB will receive inadequate treatment for several weeks or months before the correct diagnosis is made and an appropriate treatment is started. The consequence is that many MDR-TB patients will have a prolonged period of infectiousness and be a danger to other patients and to the staff. Furthermore, as the cure rate of patients with MDR-TB strains is lower than the cure rate in patients with sensitive strains, some patients with MDR-TB can become chronic excretors (the author has observed a case surviving 27 years with a smear-positive pulmonary TB resistant to all anti-TB drugs known in the 1970s).
Infectiousness and Transmission of MDR-TB Strains
The problem of the duration of the infectious period of patients with drug-resistant forms of TB is debated.31 Animal models do not confirm the impression of a higher risk of transmission from drug-resistant TB cases32 and the sputum positivity is not always correlated with the infectiousness.33 In spite of this, many MDR-TB cases seem to have been acquired in a hospital9 and infection-control measures should be considered with special attention in all settings where patients with MDR-TB are treated, in order to decrease the risk of transmission to other patients, visitors or healthcare workers.34 A recent survey has demonstrated that, even in Europe, the current management of MDR-TB and XDR-TB, and in particular the infection-control measures, is far from optimal.35 Active case finding among the contacts of patients with MDRTB should be performed to detect the presence of other cases in the same social group. It is particularly important to assess if children with MDR-TB have been in contact with relatives with a similar form of TB.
Once the strain has become resistant to one or several drugs, it can be transmitted to contacts who may develop a similar disease without having been submitted to any previous error in management.36 MDR-TB can be observed in patients who were never treated before and were infected by another case of MDR-TB (primary forms) or in patients who already received some form of drug treatment for tuberculosis and interrupted, relapsed or failed the first treatment attempt (secondary forms). The proportion of primary forms in a population reflect the current deficiencies of the programme to prevent the transmission of tuberculosis, whereas the secondary forms result from prior errors during the management of cases who received an incomplete or inappropriate treatment schedule.
The clinical forms of MDR-TB are similar to the forms due to drugsensitive strains. The clinical presentation may be more severe, with extensive lesions, if the correct diagnosis and initiation of an appropriate treatment was delayed.
Treatment of MDR-TB
The emergence of M. tbc strains resistant to anti-TB drugs has been described as occurring rapidly after the introduction of streptomycin37 and led to the concept of drug combination for the treatment of tuberculosis.1 Until the 1990s and the rapid emergence of MDR-TB in New York,38 the treatment was mainly empirical, with unsatisfactory results (44 % death or failure in the report by Goble in 199339), until some attempts in standardisation were published, mostly relying on expert opinion.40 Then, some of the basic principles of management of drug-resistant tuberculosis, like the rule of not adding a single drug to a failing regimen, have been defined, but were largely ignored by physicians in many regions of the world.
The first Guidelines on the management of drug-resistant tuberculosis, including MDR-TB, were published by the WHO in 1996.41 The proposal was to administer 3 months of a combination of five drugs, always containing at least one injectable drug and a quinolone, followed by three oral drugs administered during 18 months. The Guidelines were revised in 2006 and 2008,42 followed by a field guide in 2009.43 A complete revision was published in 201144,45 and a new companion handbook in 2014.46 Other Guidelines or recommendations have been published by the International Union against TB47 and by the Tuberculosis Network European Study Group TBnet.14 The rationale behind the new recommendations of WHO, which are more or less similar to other proposals from the recent literature,48 is to treat the patient with the drugs that offer the highest possible prospect of rapid bactericidal action and to treat long enough to be certain to eradicate the last existing mycobacteria.
The current recommendations of WHO2,44 for the treatment of MDR-TB
include the following points:
- Rapid DST for isoniazid and rifampicin or at least of rifampicin alone,
as a proxy for MDR-TB, in all cases suspect of MDR-TB (this may be all
cases in some regions of the world). - The treatment regimen should include four drugs with proven or likely
effectiveness in the intensive phase, including an injectable drug,
later-generation fluoroquinolone (no ciprofloxacine), ethionamide or prothionamide, and either cycloserine or para-aminosalicylic
acid (PAS). - The recommended duration of the intensive phase is now 8 months,
followed with at least 12 months of continuation therapy (after
termination of the use of the injectable drug). - Monitoring the response to MDR-TB treatment with smear and cultures.
- Addition of antiretrovirals in patients co-infected with HIV.
- The management of MDR-TB should be based mainly on ambulatory
care and not hospitalisation, in order to limit the possible transmission
to other patients, healthcare staff and visitors. Outpatient management
needs the implementation of a well-functioning network of community
workers and decentralisation of care close to the patient’s residence
The recommendations from WHO are based on the existing evidence, but there are still very few studies comparing different regimens and treatment options. The outcome of treatment as reported in observational studies and in the last WHO report is currently unsatisfactory,49,50 with a success rate of about 50 % (documented cure or treatment completion), below the success rate for drug-sensitive TB. Interestingly, one of the only studies comparing several treatment options demonstrated that a high success rate (89.7 %) can be obtained by a 9-month regimen, including gatifloxacin, clofazimine, ethambutol and pyrazinamide throughout the treatment period supplemented by prothionamide, kanamycin and highdose isoniazid during the intensive phase.51 These results were confirmed by a large study of more than 500 patients in Bangladesh and by several studies in Africa.52–54 Omitting the quinolone or the high-dose isoniazid or presence of a resistance to quinolones gave a lower rate of success. Although these results may not apply to other settings, particularly Eastern Europe with high rates of additional resistance, and gatifloxacine is not authorised in many countries, the results are interesting and demonstrate that the cure rate may be high, even with a shorter regimen. Further studies are currently ongoing to confirm these findings.
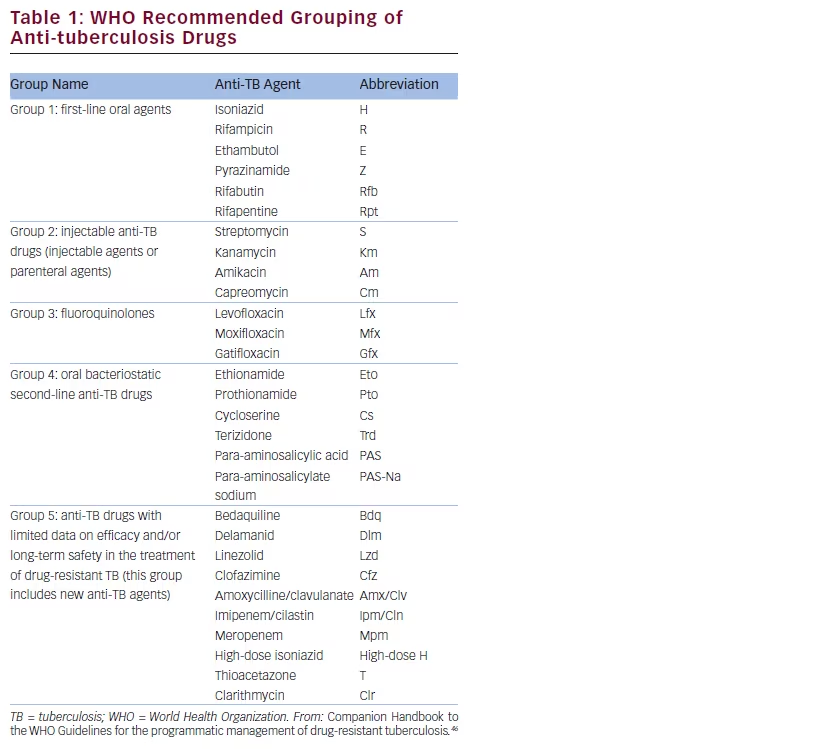
The list of second-line drugs, which may be used for the treatment of MDR-TB and XDR-TB, is presented in Table 1 (after WHO).2 Among the first-line drugs, isoniazid and rifampicin are considered inactive by definition and will not be used, but some experts recommend the use of isoniazid in higher doses, due to the fact that the resistance to isoniazid may not be complete.55 The results from the study in Bangladesh seems to confirm this option.51 The latest recommendations from WHO also propose to keep pyrazinamide in the treatment schedule, considering that the DST for pyrazinamide is not fully reliable and is not available in many laboratories.
Administering moxifloxacine in a normal or increased dose, in spite of resistance to quinolones, seems to improve the outcome, if the strain has retained an intermediate sensitivity.56
Several studies have demonstrated that linezolid is a potent antituberculous drug with good efficacy against most MDR-TB strains, but the use is limited by high costs and high frequency of adverse events.57,58 Clofazimine, an anti-leprosy drug, is another drug with a potential efficacy against drug-resistant TB strains, and has been used in a 9-month regimen in Bangladesh, but the experience is still limited, the drug is not available in all countries and has not been approved for the treatment of TB.59,60
Other drugs with weak activity, such as meropenem, co-trimoxazole, clarithromycine, co-amoxycilline and thioridazide, may be considered in cases where the number of available drugs with proven activity is limited, particularly in cases with XDR-TB.61
The treatment of MDR-TB and XDR-TB is long, difficult, expensive and associated with a high rate of adverse events (up to 79 % in some reports).62,63 The correct use of second-line drugs requires experience and a good knowledge of their effect and interactions.64 Some adverse events will necessitate the addition of other drugs, increasing the number of drugs to be used and the cost of treatment. The costs of treatment of MDR-TB are much higher than the costs of treatment for drug-sensitive TB. In countries with limited resources or in regions where MDR-TB are a large proportion of all cases, the costs to a national TB programme may not be affordable.65
Surgery, which was one of the only options for cure before the antibiobic era, is again mentioned as one option in the framework of the treatment of drug-resistant TB. Its place has recently been revised.66–68 In patients with a new episode of MDR-TB, unilateral lung involvement and good general condition, surgery seems to improve the outcome whereas in patients in retreatment, with XDR-TB, bilateral disease or low body mass index, the outcome is poor.
Drug-resistant stains can be transmitted to contacts. The evidence of the benefit of a preventive treatment for infected contacts is limited, but some studies seem to support a policy of preventive treatment according to the pattern of drug resistance of the index case.69,70
New Options
The current treatment options for MDR-TB are far from satisfactory, but are presently the best hope for a cure. New, more efficient, drugs have been recently introduced and may allow in the future an increase of the cure rate and a decrease of the duration of treatment. Recently, encouraging reports were published on the efficacy of delamanide (OPC67683),71,72 bedaquiline (TMC207)73 and pretonamid (PA-824),74 which all have the potential of shortening the time to culture conversion and to improve the outcome. The WHO has issued policy documents on the use of bedaquiline75 and delamanid,76 but the new drugs have been approved in few countries only and the experience with them is still limited. QT prolongation induced by the new anti-TB drugs and by the combination with several other drugs, like quinolones and clofazimine, is a matter of concern and makes regular monitoring mandatory.77 Errors in the use of the new drugs may increase the size of the problem in the populations, like the improper use of rifampicine after its introduction, which probably led to the development of MDR-TB. Therefore, the new drugs will have to be used under strict conditions, bearing in mind the potential negative consequences of further errors in management.
Prevention of MDR-TB
As long as there is no rapid, cheap and efficient treatment for MDR-TB, the best hope for the control of the problem is the prevention of the transmission of resistant strains in the population and the correction of errors, which may induce an increase or an extension of the MDR-TB strains.78,79 The conditions for this, as detailed in a recent report from WHO,80,81 are:
- The rapid detection of drug-resistant strains among all cases of
tuberculosis, particularly among patients with relapse, failure or
risk factors for resistance or among patients exposed to MDRTB
in their environment. This needs a well-functioning network of
laboratories with the capacity for performing rapid DSTs. The use of
the new molecular genotyping analysis (like MTB-RIF assays) have
demonstrated a potential for shortening the delay of detection of
drug resistance,82-84 but there are financial obstacles to the broad
implementation of such devices, particularly in places where they
would be most needed. In the meantime and in the places where
rapid technologies are not in place, it is the responsibility of the local
TB programme managers (and the health authorities) to ensure that
the more traditional methods are used in an efficient way, avoiding
interruption in consumables delivery, use of inappropriate procedures
and long delays in the transmission of the results to the clinicians. - The appropriate treatment of all cases with proven or suspect drug
resistance, in order to avoid the creation of further drug resistance
(amplification phenomenon) and reduce the period of infectiousness
and the duration of possible transmission to a minimum. - Infection control measures, to limit the transmission of M. tbc strains
to healthcare workers, other patients and visitors. - The availability of quality-controlled second-line drugs, without
interruption in drug delivery, stock-outs, administrative or financial
obstacles. - Proper case management until the cure of the patients, particularly
for patients with risk of treatment interruption for any reason
(deportation, imprisonment, travel, refusal, conflicts with local
managers). If needed, decentralisation of care to facilitate the
adherence has to be considered.85 As stressed by members of the
International Union against TB, ”a poor drug-resistant programme is
probably worse than no programme at all”.86
The Future
MDR-TB and XDR-TB are serious threats to the control of tuberculosis in many regions of the world, apart from HIV, and frequently simultaneously with it. They are an obstacle to the intended policy of TB elimination.87,88 New drugs89 may improve the outcome in the future, but need to be approved and available in the countries that need them most. New vaccines90 may help to control the situation, but there is no real prospect for them in the near future.91 Therefore, the best current option is an improvement of preventive measures, by a proper implementation and use of the diagnostic methods, careful selection of the appropriate treatment, efforts to obtain the cure of all new cases and infection control to avoid the further extension of the disease in the population.92 If we fail, there may be a return to ancient times, where the cure of tuberculosis was mainly left to chance, sunlight, cod liver oil and bed rest in sanatoria.93